
2026-01-18
Three months ago, a 27-year-old man, Mr. Wu, walked into the office of Dr. Cao Quanfu, Director of the Andrology Department at Shenzhen Hengsheng Hospital's Reproductive Medicine Center. He carried a devastating diagnosis: "Severe Oligoasthenospermia." Engaged to be married, Mr. Wu was filled with anxiety and urgency. Previous doctors had suggested he explore in vitro fertilization (IVF), leaving him unsure if biological fatherhood was still possible.
Mr. Wu's condition, clinically termed severe oligoasthenospermia and commonly known as "dead sperm" syndrome, presented a grim picture: not only was his sperm count extremely low, but under the microscope, virtually no motile sperm could be found. Traditional treatments offered limited hope. Even with IVF, there was no guarantee of retrieving enough viable sperm for a biological child, potentially leaving donor sperm as the only option.

Left image: Sperm motility trajectories from Mr. Wu's analysis
However, Dr. Cao believed low count and poor motility were merely symptoms. The key was to find the underlying cause. Instead of immediately opting for IVF, Dr. Cao initiated a comprehensive diagnostic workup for Mr. Wu.
Precise Diagnosis: Identifying the "Roadblock"
Mr. Wu fully cooperated with a series of examinations. Soon, high-definition ultrasound revealed the truth: the problem was a physical obstruction in the sperm transport pathway. Imaging clearly showed an abnormal cystic lesion in his seminal vesicle region. This "roadblock" was compressing the ejaculatory duct, causing a partial obstruction. Sperm struggled to pass, leading to long-term stagnation, oxygen deprivation, and ultimately, loss of motility and massive sperm cell death. The issue wasn't that Mr. Wu's sperm were inherently defective; they were effectively being "suffocated" by the blockage.
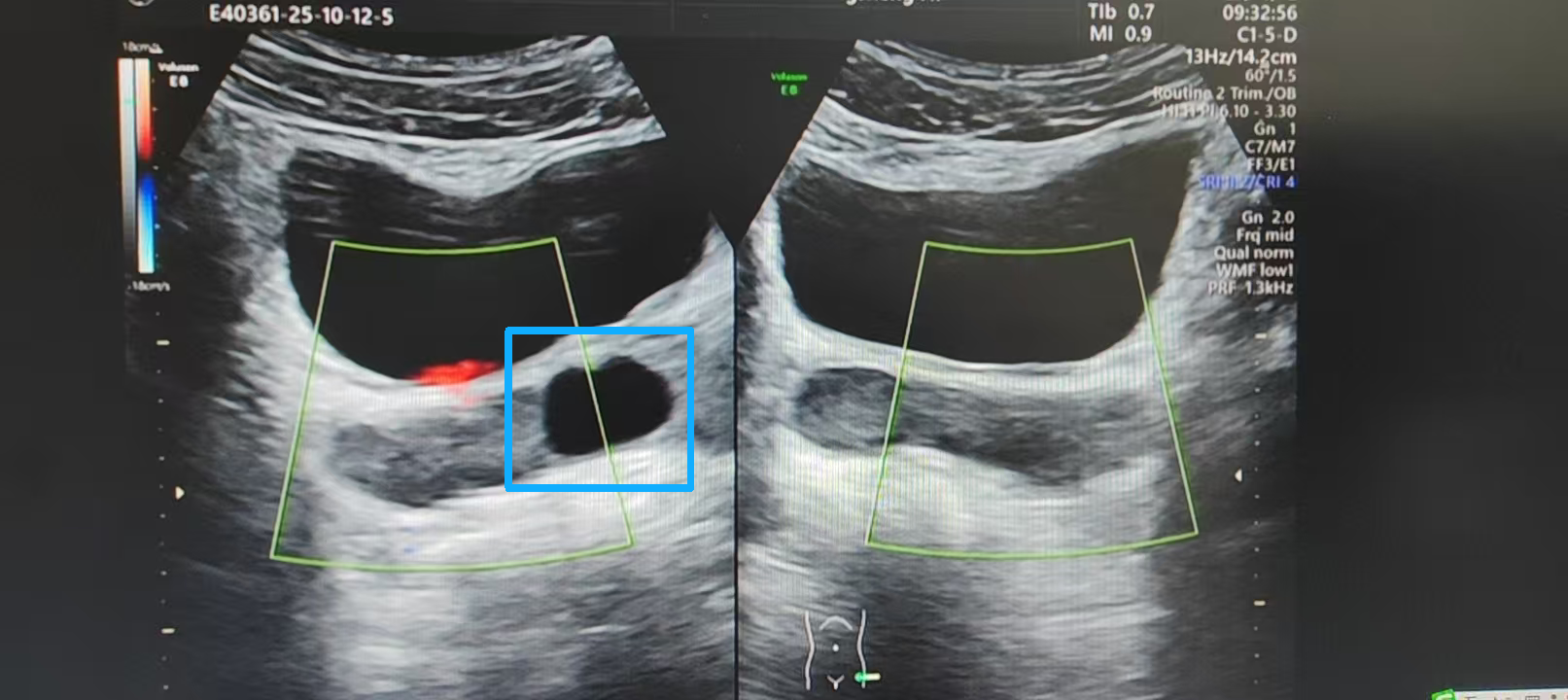
Ultrasound image showing the cystic lesion (outlined in blue)
A One-Hour Minimally Invasive Solution
With the cause identified, a targeted solution was possible. The andrology and urology team designed a minimally invasive procedure for Mr. Wu: Transurethral Seminal Vesiculoscopy with Ejaculatory Duct Dilation.
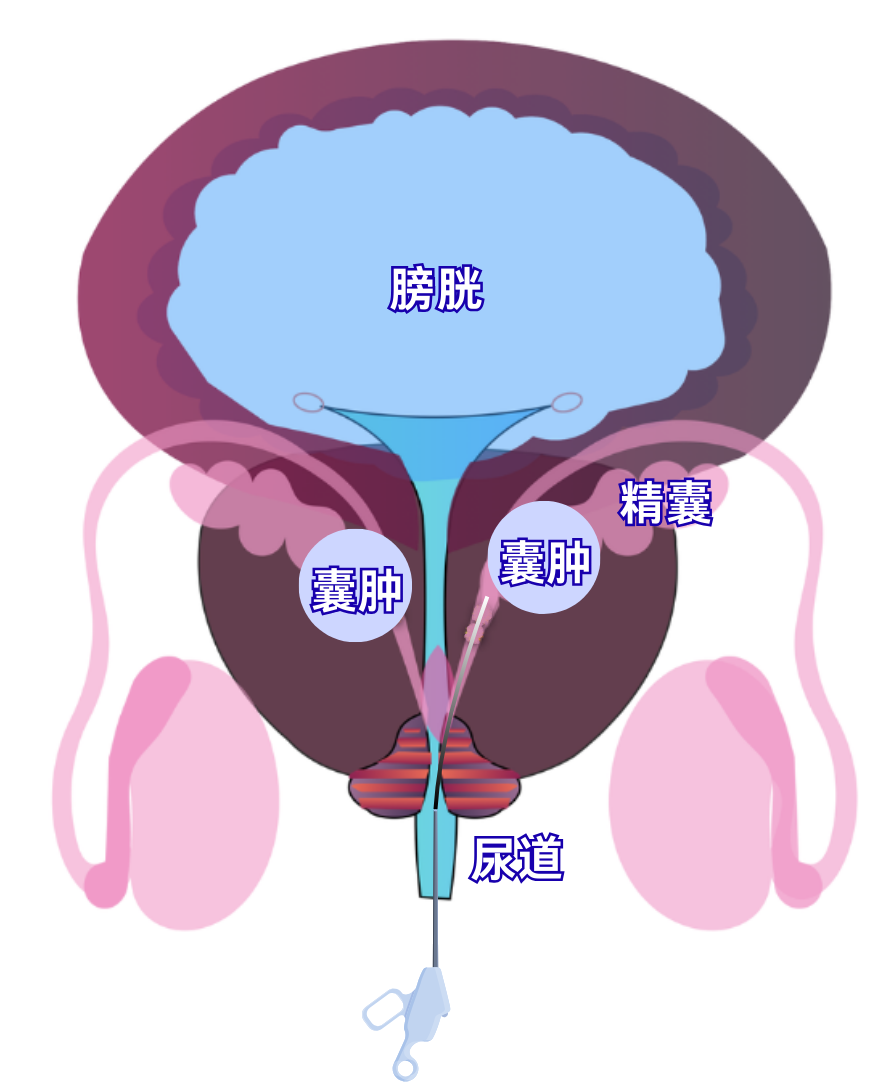
Surgical procedure schematic
Using a slender endoscope inserted through the natural orifice (the urethra), surgeons navigated directly to the affected area. Under direct visualization, they relieved the cyst's compression on the ejaculatory duct and dilated the narrowed lumen. The entire surgery took just one hour. Mr. Wu's total hospital stay was five days.
Postoperative Miracle: From "Static" to "Active"
The speed of recovery was astonishing. The first post-operative semen analysis showed a normalized total sperm count and, critically, the presence of progressively motile sperm under the microscope. The "life passage" was clear. Two months later, a follow-up analysis delivered even more encouraging news: all key parameters for sperm count and motility had returned to normal ranges.
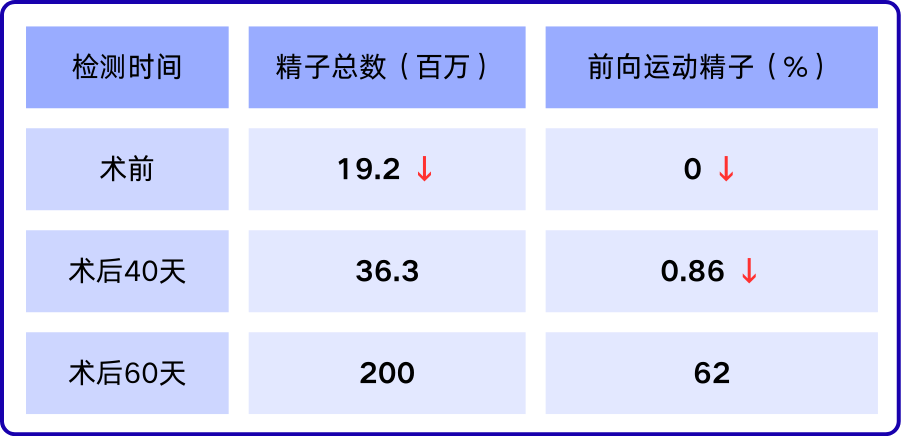 Comparison of Mr. Wu's pre- and post-operative semen analysis results
Comparison of Mr. Wu's pre- and post-operative semen analysis results
This meant Mr. Wu had regained his natural ability to conceive. He could now look forward to marriage and fatherhood like any healthy man.
Lessons Learned: The "Detour" and the "Direct Path"
Mr. Wu's journey from a seemingly "untreatable" diagnosis to renewed hope for natural conception offers a vital lesson. In male infertility, especially cases of obstructive azoospermia or severe oligoasthenospermia, precision diagnosis is the crucial first step. Modern andrological surgery can now resolve with minimally invasive techniques what was once considered hopeless.
A common response to cases like Mr. Wu's is often: "Natural conception is impossible. Proceed directly to surgical sperm retrieval (TESA/PESA) for Intracytoplasmic Sperm Injection (ICSI, or 'second-generation IVF')." While IVF/ICSI can be a vital path to parenthood, it may become an unnecessary "detour" if pursued without first identifying a treatable obstruction.
Dr. Cao emphasizes that while Assisted Reproductive Technology (ART) like IVF is a powerful tool, it should be viewed more as a "final rescue mission." For Mr. Wu, hastily choosing ART would have meant higher physical, financial, and psychological burdens, potentially leaving him with the lasting stigma of "infertility."
Dr. Cao's reminder to men facing fertility challenges is clear: male infertility has complex causes. Do not give up based on a single report. Through precise andrological surgical intervention, many men who have been handed a "fertility death sentence" can reclaim the joy of natural conception.

Deputy Chief Physician. Expert in a multidisciplinary approach to male infertility, integrating urology, reproductive medicine, and andrology. Offers unique insights into male infertility, ART, reproductive health, and sexual dysfunction. A national leader in treating azoospermia, oligoasthenospermia, and related conditions.
Free Consultation
