
2025-11-13
In the field of precision cancer therapy, every 0.1-millimeter breakthrough can rewrite the script of life.
When middle-aged Ms. Li (a pseudonym) received her diagnosis, she felt lost and helpless – it was moderately differentiated adenocarcinoma of the sigmoid colon with multiple liver metastases (cTxNxM1b Stage IVb). A massive tumor, approximately 18.06 x 12.6 cm, had already been growing aggressively in her right liver, like a time bomb.
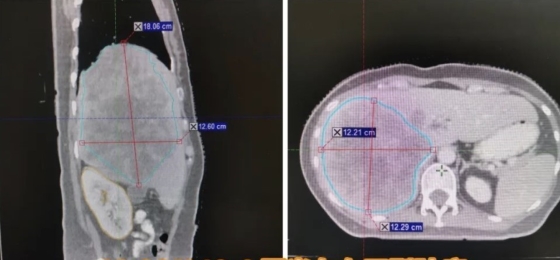
Faced with the limitations of conventional treatment options, Ms. Li sought out the team of Director Chen Bingguang, an expert in abdominal and pelvic sarcoma at the Foshan Chancheng Hospital Tumor Center. By employing innovative radiotherapy technology and conducting an International Multidisciplinary Team (MDT) consultation, they charted a path to rebirth for Ms. Li: a strategy of "'precision radiotherapy combined with chemotherapy + targeted therapy' as conversion therapy".
01 Precision Radiotherapy with SCART Technology Tackles the Giant Tumor
Director Chen's analysis: Ms. Li's giant tumor posed a significant challenge. Surgical specialists assessed that the tumor invaded multiple major blood vessels, including the portal vein, hepatic veins, and inferior vena cava, rendering it inoperable. Conversion therapy was needed to possibly create a chance for surgery. However, standard conversion therapy relies solely on chemotherapy combined with targeted therapy, which offers some opportunity for patients with smaller tumors and less extensive vascular invasion. For a patient like this, with a liver metastasis reaching 18 cm and involving multiple major vessels, the chance of successfully controlling and shrinking the tumor enough for surgical resection was minimal.
How to break through this impasse? The patient's strong will to live and her full trust in the experts led Director Chen to boldly propose his idea: Could radiotherapy be delivered concurrently with conventional chemotherapy + targeted therapy to enhance tumor shrinkage? Reviewing the literature revealed no relevant reference data for this new treatment model in such cases. Furthermore, when facing a giant tumor exceeding 10 cm in diameter, radiotherapy often faces a dilemma: colorectal cancer is not very sensitive to conventional radiotherapy, yet liver tissue is highly sensitive to radiation. Increasing the dose risks causing severe liver damage, while reducing the dose is like scratching an itch from outside the boot.
Director Chen proposed using Stereotactic Central Ablative Radiation Therapy (SCART) technology to achieve precise targeting of the giant tumor. This innovative technique, integrating Stereotactic Body Radiotherapy (SBRT) with Spatially Fractionated Radiation Therapy (SFRT), is primarily used to treat recurrent or metastatic giant tumors.

Director Chen analyzing the condition and treatment plan for a patient (not the patient in this case)
SCART technology can precisely and safely deliver ablative radiation doses to the stubborn core area of the tumor, achieving precise delivery of ablative-level high doses to the tumor core, while providing a rapid dose fall-off to protect surrounding tissues, thereby effectively controlling tumor growth.
SCART technology can precisely and safely deliver ablative radiation doses to the stubborn core area of the tumor, achieving precise delivery of ablative-level high doses to the tumor core, while providing a rapid dose fall-off to protect surrounding tissues, thereby effectively controlling tumor growth.
02 Three-Step Comprehensive Treatment Plan
Following the recommendations of Director Chen and the international MDT team, Ms. Li's treatment plan proceeded in three steps:
Step 1: First, target the giant liver mass with SCART radiotherapy (PTVm1 15Gy/3f, STVm1 72Gy/3f). This delivered ultra-high doses precisely to the tumor core. Just three treatment sessions achieved a biological effect comparable to what would traditionally require 33-35 fractions over three courses. Concurrent chemotherapy + targeted therapy for 4 cycles created a dual attack of "local ablation + systemic control," leading to tumor volume reduction and significant relief of compression symptoms.
Step 2: Target the substantially reduced residual tumor with a second course of SCART radiotherapy (PTVm1C2 15Gy/3f, STVm1C2 63Gy/3f), further shrinking the tumor to create conditions for surgery, transforming the status from "unresectable" to "operable."
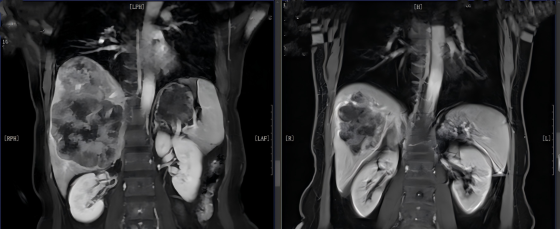
The 18-cm giant tumor gradually shrank to 6.4 x 4.9 cm under the "one-two punch" of precision medicine and chemotherapy + targeted therapy, allowing the patient to subsequently qualify for surgical resection. This could increase the patient's 5-year survival rate dramatically from the 5-10% associated with inoperable disease to 40-60%, significantly improving both survival time and quality of life, even offering the possibility of long-term disease-free survival.
Step 3: Progressively complete radical resection of the intestinal and liver tumors, followed by subsequent systemic therapy.
The success of Ms. Li's case highlights the medical team's responsibility and commitment to "addressing the patient's urgency." Faced with a patient in a desperate situation, they were willing to take risks and innovate. Driven by the belief and determination to "not give up on any cancer patient," they secured a greater possibility of a cure for her.
Simultaneously, it confirms the ability of SCART technology to push the boundaries of traditional precision radiotherapy. It further reveals the essence of modern cancer treatment: using the precision of technology to ablate disease, and warming lives with the wisdom of collaboration and the compassion of healers, rekindling the light of hope for more patients with advanced cancer.

