
2025-11-04
Having previously suffered from surgery, he was absolutely opposed to going under the knife again after being diagnosed with "golden cancer" – prostate cancer! As a pillar of society and a highly educated professional, determined to preserve his male dignity and avoid social embarrassment, he resolutely chose CyberKnife radiotherapy in Foshan. Two years post-treatment, he is now...
01 PSA levels continue to rise - prostate cancer!
A 56-year-old male, Mr. Li (a pseudonym), underwent a routine checkup which revealed an elevated PSA value of 5.12 ng/ml. Following his doctor's advice, he regularly monitored his PSA levels to observe the trend.
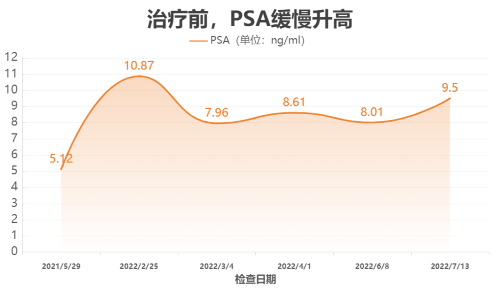
Unexpectedly, from May 2021 to June 2022, Mr. Li's PSA levels gradually increased. Further investigation via prostate MRI and biopsy confirmed the diagnosis: High-Risk Prostate Cancer; T2b, N0, M0; Gleason Score 4 + 4 = 8 (ISUP Grade Group 4). Local doctors recommended prompt surgical intervention.
PSA, or Prostate-Specific Antigen, is regarded as a barometer of male prostate health. PSA normally exists at very low levels in the blood, with a typical normal value <4 ng/mL. However, when prostate cancer develops, PSA levels can rise significantly, often exceeding 10 ng/mL, making PSA an important indicator for the early detection of prostate cancer.
02 Consulting Director Han, Seeking a Non-Surgical Approach
Faced with the prospect of surgery, Mr. Li hesitated. This was because in July 2021, he had undergone a wedge resection and segmentectomy of the left upper lung for lung cancer. The pain experienced during and after that surgery, and the recovery period, still haunted him. He strongly hoped to find a non-surgical treatment method.

With this in mind, and upon a friend's recommendation, Mr. Li sought out Director Han Liangfu, an expert specializing in prostate cancer radiotherapy at the Foshan Fosun Chancheng Hospital Tumor Precision Diagnosis and Treatment Center. Based on the patient's individual circumstances, comprehensive prostate PSMA PET/CT results, and international guidelines, Director Han provided a detailed analysis of the condition and offered two treatment options for consideration.
03 Radiotherapy and Surgery are Comparable, with Differing Side Effect Profiles
Director Han stated:
According to the MSKCC pre-prostatectomy prediction calculator, the patient's data indicated the following predicted probabilities: 69% for extracapsular extension, 22% for pelvic lymph node involvement, and 13% for seminal vesicle invasion.
The ProtecT study compared the long-term efficacy of active monitoring, surgery, and radiotherapy for prostate cancer. 1,643 cases (primarily low-risk, some intermediate/high-risk) were randomized to active monitoring (PSA testing every 3 months in the first year, then every 6-12 months), radical surgery, or radical radiotherapy (74Gy/37 fractions) + 3-6 months of neoadjuvant and concurrent androgen deprivation therapy (ADT). The 10-year follow-up results showed: disease-specific survival rates were 98.8%, 99%, and 99.6% respectively. Cases of metastasis were only 33, 13, and 16 respectively. The surgery group experienced significant impacts on sexual function and urinary continence, while the radiotherapy group had higher gastrointestinal reactions, most apparent at 6 months but gradually recovering thereafter.
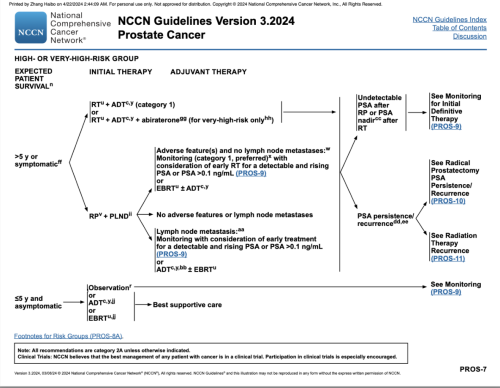
NCCN Guidelines for Prostate Cancer Treatment.
In summary: The patient could choose either radical prostatectomy + pelvic lymph node dissection +/- post-operative radiotherapy, or external beam radiotherapy (EBRT) combined with long-term (18-24 months) androgen deprivation therapy (ADT). Radiotherapy and surgery offer comparable efficacy, with differing side effect profiles.
04 PSA Drops, Tumor Disappears After 5 Radiotherapy Sessions
Director Han discussed the treatment details, potential side effects, and precautions thoroughly with the patient. After considering for just one day, the patient and his family decided on the non-surgical option, choosing Linear Accelerator-based Stereotactic Body Radiotherapy (SBRT) combined with long-term Androgen Deprivation Therapy (ADT).
Considering no pelvic lymph node metastasis was detected, Director Han defined the radiotherapy target as the prostate and part of the seminal vesicles. The dose fractionation was set at 7.25Gy per fraction for 5 fractions.
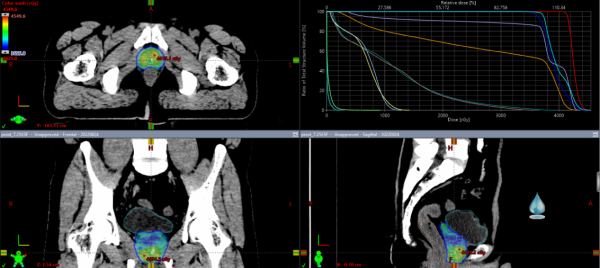
The radiation target was defined as the prostate and part of the seminal vesicles, sparing other healthy tissues.
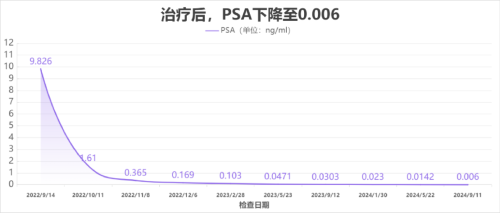
After completing the 5 radiotherapy sessions, the patient reported no discomfort; his PSA level had returned to the normal range by October 2022.
Over the subsequent two years, with continued ADT and PSA monitoring, his levels remained near zero. This signifies that the threat from Mr. Li's prostate cancer has essentially vanished, the results are evident, and his quality of life is excellent.
Mr. Li and his family are very satisfied with this outcome. Precise radiotherapy allowed him to avoid the numerous potential complications of surgery and the awkwardness of the recovery period. Using precise radiotherapy and medication alone, he achieved results comparable to surgery.
More importantly, the disease was treated without damaging healthy tissues, preserving male dignity, and without impacting his daily social life.
Potential acute and long-term side effects of radiotherapy include, but are not limited to, the following:
① Acute reactions may commonly include fatigue, increased urinary frequency, slower urine stream, reduced tension; possibly increased bowel movement frequency, aggravated hemorrhoid symptoms; less commonly, blood in stool, rectal tenesmus, pain, burning during urination, difficulty urinating; rarely, diarrhea or difficulty defecating; very rarely, decreased blood cell counts.
② Long-term chronic reactions may commonly include decreased sexual function, less sustained erections, infertility; less commonly, blood in stool, chronic diarrhea, difficulty urinating, straining during bowel movements, etc.; very rarely, severe chronic diarrhea, blood in urine, rectal or urinary tract ulceration/bleeding potentially requiring surgical intervention, radiation-induced secondary primary cancer, etc.

