
2025-11-04
Starting last December, Ms. Zhang experienced nasal congestion and a runny nose. Thinking it was the flu, she took cold medicine for a few days. When her symptoms improved slightly, she didn't think much of it. However, after over a month passed, her nasal discharge became thicker. It was then that she decided to see a doctor. A nasal endoscopy revealed a nasopharyngeal mass; combined with MRI and pathological biopsy, she was diagnosed with: Malignant Tumor of the Nasopharynx T1N2M0 Stage III.
Extremely worried and anxious, Ms. Zhang sought out experts and hospitals renowned for treating nasopharyngeal carcinoma (NPC), eventually finding Director Lu Qiuxia, a head and neck specialist at the Foshan Chancheng Hospital Tumor Precision Diagnosis and Treatment Center.

Director Lu during a consultation
Subsequently, a detailed PET/CT scan indicated: a hypermetabolic space-occupying lesion in the nasopharynx; mildly enlarged lymph nodes in bilateral neck areas with increased metabolism, highly suggestive of metastasis.
"Nasopharyngeal carcinoma is relatively sensitive to radiotherapy; concurrent chemoradiotherapy can be considered," Director Lu reassured Ms. Zhang. "Radiotherapy is relatively easier than surgery. There's no incision and no pain, so there's no need to worry too much."
Ms. Zhang underwent concurrent chemoradiotherapy: For the nasopharyngeal site, Volumetric Modulated Arc Therapy (VMAT) was used, delivering 69 Gy in 30 fractions. This was synchronized with 2 cycles of chemotherapy using the Cisplatin 100mg/m² regimen.
At a follow-up just one month after completing radiotherapy, Ms. Zhang received excellent results: The tumor in the nasopharynx had basically disappeared, and her nasal congestion and runny nose symptoms had significantly improved.
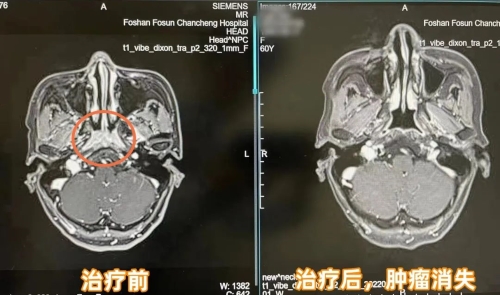
Comparison of Ms. Zhang's medical images before and after treatment.
Ms. Zhang and her family found the entire treatment process very comfortable and were pleasantly surprised by the outcome. Their words were full of praise and gratitude for the Foshan Chancheng Hospital Tumor Center team.

Heartfelt Thanks
Nasopharyngeal Carcinoma's Preference for "Cantonese People"
Nasopharyngeal carcinoma (NPC) is a rather unique disease, with distinct racial, regional, and familial clustering in its incidence, predominantly affecting people of Mongoloid descent. Fifty percent of the world's NPC cases occur in five southern provinces of China: Guangdong, Guangxi, Hunan, Fujian, and Jiangxi. Therefore, this cancer requires vigilance among residents originating from these southern regions of China.
Among these, Guangdong has the highest incidence rate in the world, earning NPC the nickname "Guangdong Tumor." NPC is most common in individuals aged 30-60, with the incidence rate in males being about 2-3 times that in females. Blood-stained post-nasal drip and enlarged cervical lymph nodes are its common clinical symptoms.
Be Alert to These NPC High-Risk Factors!
Many NPC patients have a family history of cancer. Besides genetic factors, this may also be related to lifestyle habits and environmental factors.
01 Genetic Factors
Studies have found that 12.3% of NPC patients have a family history of NPC; 21.6% have a family history of malignant tumors. NPC shows obvious ethnic clustering.
02 Environmental Factors
Research indicates that nitrosamines are closely related to NPC. Preserved foods contain relatively high levels of nitrosamines, such as pickled vegetables and salted fish. In Guangdong, the content of nickel in the soil, water, and rice is higher than in other regions, potentially leading to an imbalance in nickel intake among the population. Higher levels of nickel have also been detected in the hair of NPC patients compared to healthy individuals. Animal experiments suggest that excessive nickel may promote nitrosamine-induced NPC.
03 EB Virus
Immunological and biochemical studies have confirmed a close relationship between the Epstein-Barr virus (EBV) and NPC.
Risks and Symptoms of NPC
In the early stages of NPC, as the cancerous tissue invades the skull base bone, nerves, and blood vessels, patients may experience intermittently occurring migraines, or pain in the vertex/occiput or neck.
When the nasopharyngeal tumor enlarges, it may cause bilateral nasal congestion. Patients might cough up blood-tinged sputum in the morning, notice blood-stained nasal discharge when blowing their nose, or experience blood-tinged post-nasal drip.
As the NPC mass blocks the opening of the Eustachian tube on the affected side, patients may experience a feeling of ear fullness and tinnitus. Worsening of the condition can damage the auditory nerve, leading to gradual hearing loss.
Most NPC patients show symptoms of enlarged cervical lymph nodes in the early stages, feeling palpable "lumps" on the neck. These enlarged lymph nodes are often misdiagnosed as inflammation. For neck masses that do not shrink after anti-inflammatory treatment, or even continue to grow rapidly—especially those that are hard in texture, have poor mobility, are multiple and fused together into a cluster, and are painless—prompt medical attention is necessary.
NPC can also cause symptoms like facial numbness and difficulty chewing. If the condition worsens and invades the optic nerve, patients may experience double vision (diplopia).
NPC is Relatively Sensitive to Radiotherapy
NPC is a malignant tumor that is difficult to diagnose in its early stages, as early NPC often has no obvious symptoms and is not easily detected.
However, like many malignancies, early detection, early diagnosis, and early treatment are key to improving patient prognosis and reducing mortality. Early-stage NPC has a very good treatment outcome, with a cure rate exceeding 90%.
The main treatment modalities for NPC are radiotherapy, chemotherapy, and immunotherapy. These approaches require different combination strategies depending on the disease stage.
Early-Stage NPC: Primarily Treated with Radiotherapy
NPC is sensitive to radiotherapy. Furthermore, the nasopharynx has a complex structure, located at the skull base near the brainstem. The cancer can spread upward into the cranial cavity or downward to neck lymph nodes, making surgical resection difficult. Therefore, radiotherapy is the primary treatment for newly diagnosed NPC without distant metastasis, and it is the main curative treatment method for NPC.
The most commonly used technique today is Intensity-Modulated Radiotherapy (IMRT). For early-stage NPC, radiotherapy alone achieves excellent results, with a 5-year survival rate of over 90%.
Locally Advanced Tumors: Comprehensive Treatment is Preferable
For locally advanced tumors, radiotherapy alone is less effective, with a 5-year survival rate of only about 60%. Therefore, chemotherapy is added to radiotherapy for comprehensive treatment.
Metastatic (Late-Stage) NPC: Systemic Therapy is Primary
The treatment for metastatic NPC is primarily systemic therapy. Currently, chemotherapy combined with immunotherapy is recommended. Of course, the treatment plan adopted will vary from person to person depending on the specific circumstances and stage of the NPC patient.

