
2025-10-19
At around 5 a.m., an ambulance rushed an 84-year-old man to Foshan Fosun Chancheng Hospital, a member of Fosun Health Group. The patient had been experiencing continuous rectal bleeding for two hours, was extremely pale, and showed a sharp drop in blood pressure. His hemoglobin level had fallen to just 50 g/L (normal range for adult males is approximately 120–160 g/L). The severe gastrointestinal bleeding posed an immediate threat to his life.
Emergency Admission: A “Life-or-Death” Alarm
Diagnostic tests revealed that the patient’s pancreatic tumor had invaded the duodenum, causing recurrent bleeding. CT imaging showed a pancreatic head tumor, pancreatic atrophy, and pancreatic duct dilation.
Given his advanced age, poor pulmonary function, and malnutrition, the surgical risk was extremely high. After thorough discussions with his family, the medical team decided on a two-step approach: first, an emergency gastroduodenal artery embolization to stop the bleeding, followed by a laparoscopic pancreaticoduodenectomy to remove the tumor—the “bleeding time bomb”.
A complex, high-risk surgery requiring multidisciplinary collaboration was about to begin.
Multi-Disciplinary Team Consultation: A Collective Effort to Solve a Surgical Challenge
Experts from the Hepatobiliary and Pancreatic Surgery Department, Anesthesiology, Surgical Intensive Care Unit (SICU), Nutrition, and Radiology departments convened a multidisciplinary team (MDT) meeting to develop a detailed and evidence-based surgical plan:
Hepatobiliary and Pancreatic Surgery Team: Responsible for tumor removal and digestive tract reconstruction, ensuring precise handling of the gastroduodenal artery and secure anastomosis.
Anesthesia and Critical Care Team: Controlled intraoperative hemodynamics and provided postoperative cardiopulmonary monitoring to minimize complications.
Nutrition Support Team: Initiated parenteral nutrition post-surgery, transitioning to enteral feeding to maintain energy balance.
Nursing Team: Implemented ERAS (Enhanced Recovery After Surgery) principles to support perioperative care.
The Surgical Battle: Precision Under the Laparoscope
The operation was led by Professor Zhong Xiaosheng from Guangdong Provincial Hospital of Chinese Medicine and Professor Zhang Haixiong from the Hepatobiliary and Pancreatic Surgery Department of Foshan Chancheng Hospital.
Using advanced laparoscopic techniques, the surgical team performed a series of precise maneuvers:
Meticulous Exploration: Carefully separated adhesions and exposed the tumor-invaded pancreatic head and duodenum, clearing the way for tumor removal.
Vascular Management: The common hepatic artery was carefully isolated and suspended to ensure its protection, and the tumor-feeding arteries—including the gastroduodenal and right gastric arteries—were sequentially ligated.
Tumor Resection: Sequentially resected from the distal stomach to the proximal jejunum, including the gallbladder, mid/distal common bile duct, pancreatic head, and the entire duodenum.
Digestive Tract Reconstruction: Reconnected the jejunum to the stomach, bile duct, and pancreas to restore digestive continuity.
Minimally Invasive Advantage: Leveraged the 3D laparoscopic small-incision approach to minimize trauma, reduce postoperative pain, and accelerate recovery.
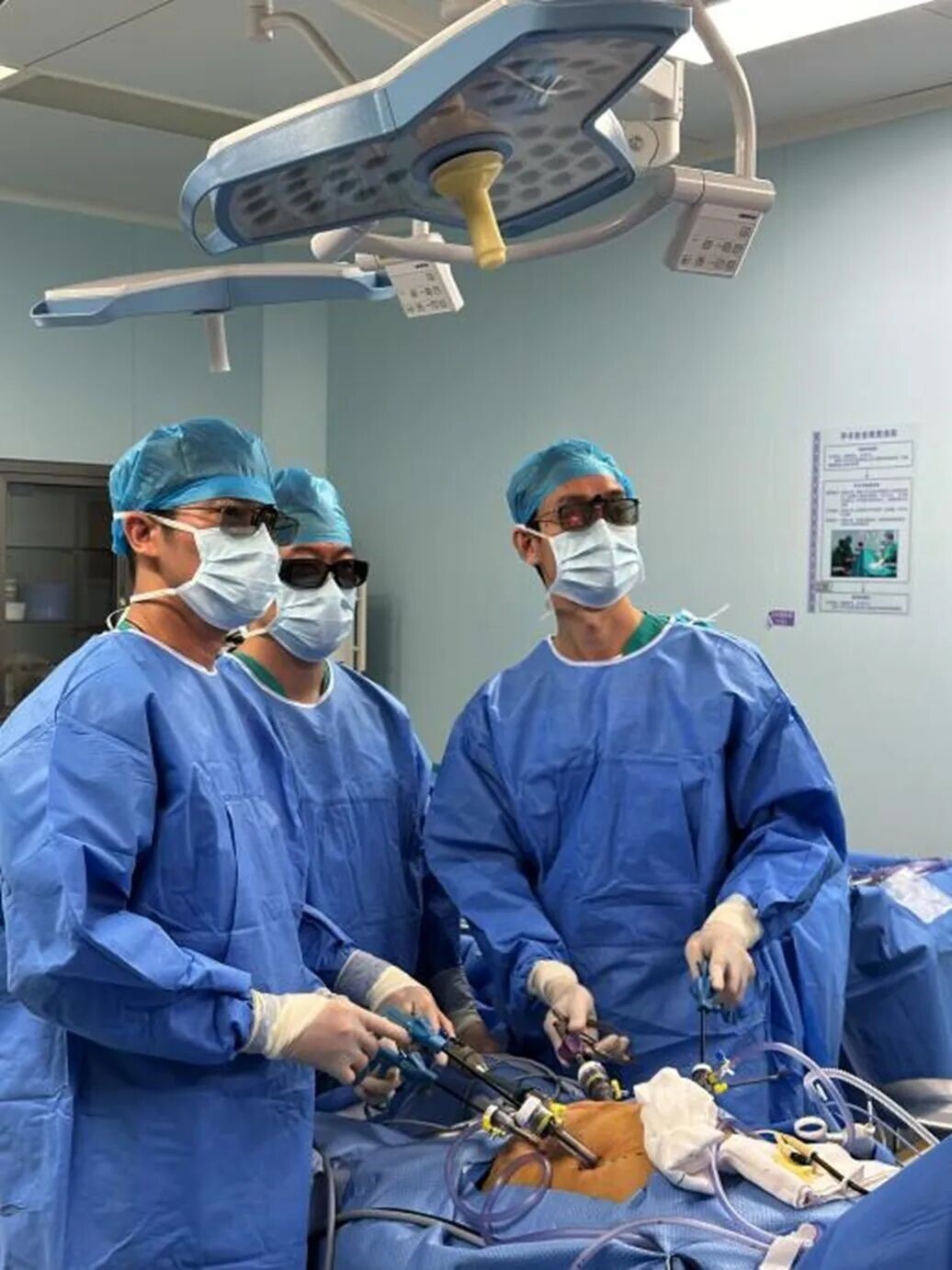
3 advanced technologies ensured surgical precision:
3D Laparoscopy: Provided a 10× magnified, high-definition view, allowing clear visualization of blood vessels and nerves.
Fluorescence Imaging: Enabled real-time tracking of the biliary tract to reduce surgical risks.
Precise Pressure Control: Maintained intra-abdominal pressure at 10 mmHg to minimize stress on the patient’s cardiopulmonary function.
Postoperative Recovery: ERAS Principles in Action
Successful surgery was only the beginning—recovery was equally critical. Guided by ERAS (Enhanced Recovery After Surgery) principles, the nursing team developed a personalized rehabilitation plan for the elderly patient:
Pain Management: Implemented a “preemptive analgesia” protocol to minimize postoperative pain.
Early Mobilization: On the second postoperative day, the patient began in-bed leg exercises such as “cycling movements”.
Nutritional Progression: By day four, he was able to get out of bed, pass gas and stool, and tolerate liquid foods such as rice soup.
The patient successfully overcame the key postoperative challenges of infection, nutrition, and thrombosis. His recovery exceeded expectations, and he was discharged in stable condition.
Expert Insight: Advanced Age ≠ Surgical Contraindication
“Thanks to modern medical advances, age alone is no longer a barrier to surgery for pancreatic cancer patients”, explained Professor Zhang Haixiong, Director of the Hepatobiliary and Pancreatic Surgery Department.
“Comprehensive preoperative assessment and multidisciplinary collaboration are crucial. In China, around 120,000 new cases of pancreatic cancer are diagnosed each year, and about 80% of patients are over 60 years old. Successful treatment depends on the seamless cooperation of multiple specialties—from preoperative evaluation to intraoperative technique and postoperative care.”
Foshan Fosun Chancheng Hospital has integrated resources from General Surgery, Intensive Care, Gastroenterology, Endoscopy, Medical Oncology, Radiology, and Pathology to establish a one-stop multidisciplinary service for digestive tract tumors. This model represents a shift toward “patient-centered, disease-focused” integrated care.

