Liver cancer refers to malignant tumors originating in the liver or starting from the liver. It is broadly classified into primary liver cancer (e.g., hepatocellular carcinoma) and secondary liver cancer (metastasis from other organs to the liver). Key risk factors include hepatitis B (HBV) and hepatitis C (HCV) infections, alcoholic cirrhosis, long-term exposure to aflatoxins, and fatty liver disease.
Liver cancer is primarily categorized into two types:
Primary Liver Cancer (originating in the liver)
Hepatocellular Carcinoma (HCC): Accounts for 75%-90% of cases. Linked to chronic HBV/HCV, alcoholic liver disease, and non-alcoholic fatty liver disease (NAFLD).
Intrahepatic Cholangiocarcinoma (ICC): 5%-10% of cases. Arises from bile duct epithelial cells; associated with liver fluke infection, bile duct stones, or primary sclerosing cholangitis.
Mixed Hepatocellular-Cholangiocarcinoma: Rare; exhibits features of both HCC and ICC.
Secondary Liver Cancer (Metastatic)
Cancers spread to the liver from other organs (e.g., colon, stomach, pancreas), accounting for 20%-30% of liver cancer cases.
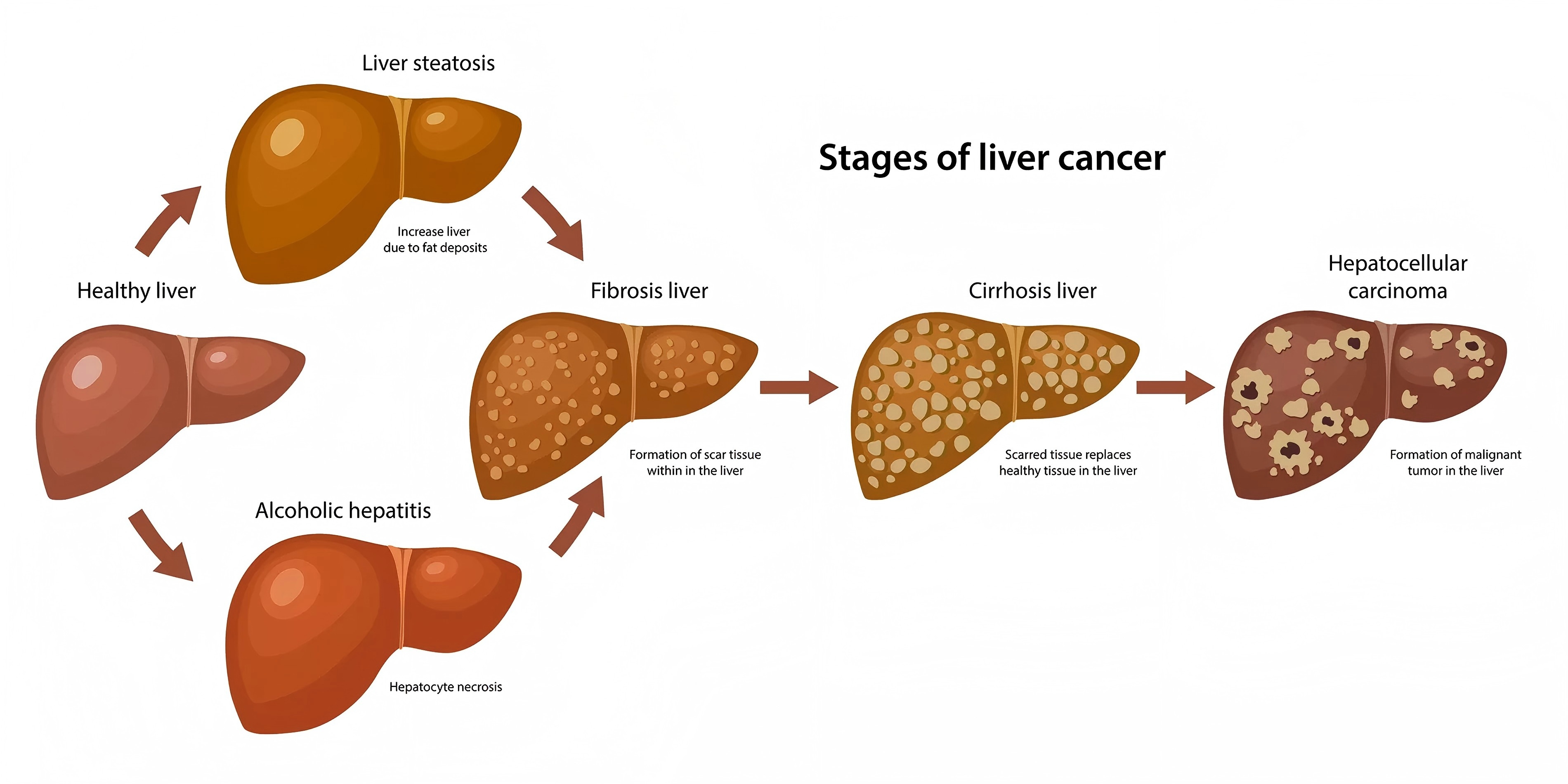
Additional Classifications:
By Morphology:
Massive type: Large solitary tumor.
Nodular type: Multiple nodular tumors.
Diffuse type: Widespread infiltration throughout the liver.
By Tumor Size:
Micro: ≤2 cm (grape-sized).
Small: 2–5 cm (walnut-sized).
Large: 5–10 cm (orange-sized).
Giant: >10 cm (melon-sized).
By Growth Pattern:
Infiltrative: Root-like invasion into surrounding tissue.
Expansile: Outward balloon-like expansion.
Mixed: Combines infiltrative and expansile features.
Diffuse: Disseminated growth across the liver.
By Cellular Differentiation (Grading):
Grade I: Well-differentiated (mature cells).
Grade II–III: Moderately differentiated.
Grade IV: Poorly differentiated (immature cells).
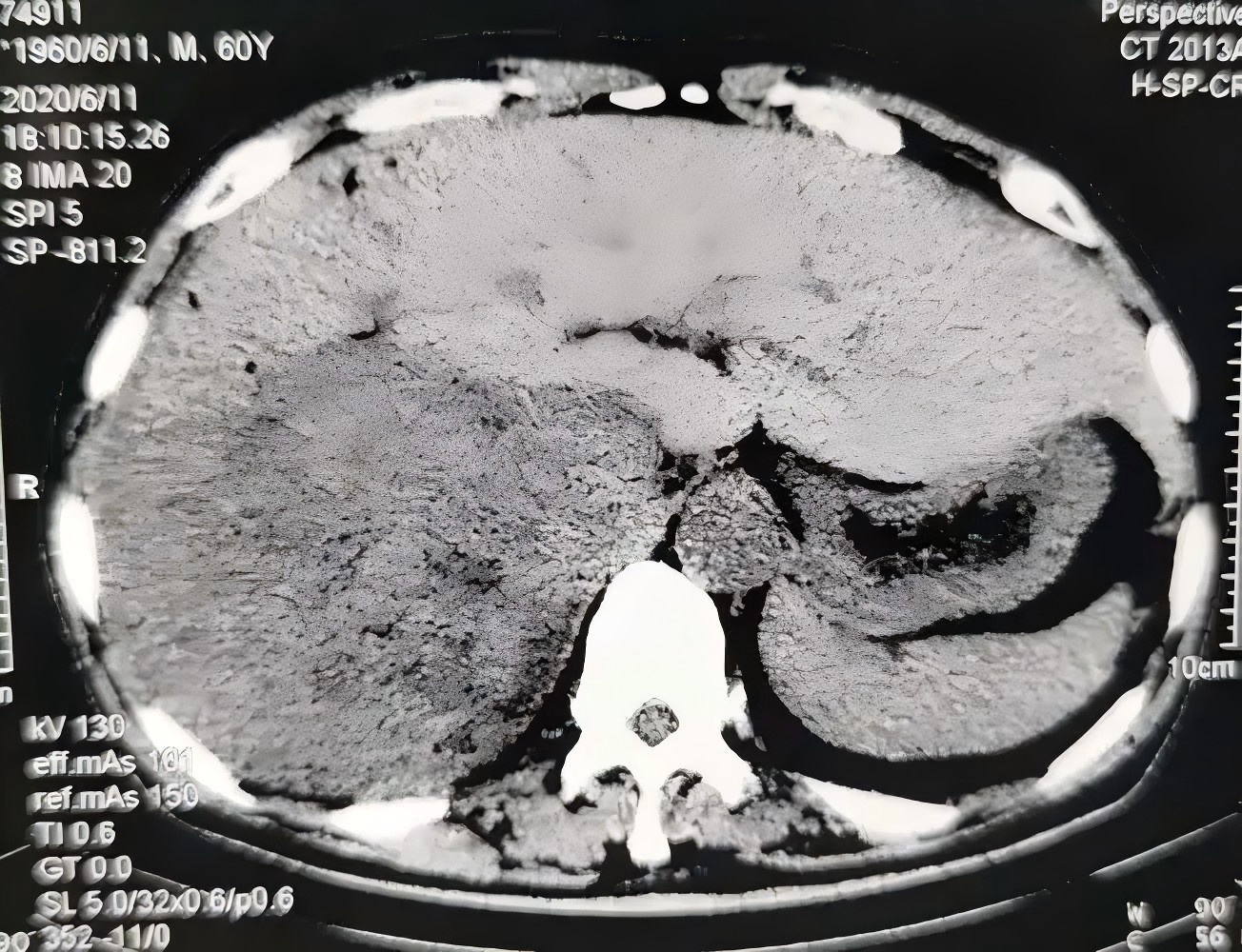
In Indonesia, liver cancer is the fifth most common cancer in both men and women. In 2022, approximately 21,000 new cases were reported (14,000 men; 7,000 women). It ranks among the top causes of cancer-related deaths, claiming nearly 19,500 lives annually, with significantly higher mortality in men. Due to late-stage diagnosis, the 5-year survival rate remains critically low at 12%–15%, highlighting urgent public health challenges.
Traditional Surgery:
Only 5–10% of advanced-stage patients qualify.
Drawbacks: High recurrence risk; large incisions; risk of vascular injury and hemorrhage due to complex liver anatomy.
Traditional Chemotherapy:
Used post-surgery to prevent recurrence.
Side effects: Immunosuppression, vomiting, hair loss, and severe weakness.
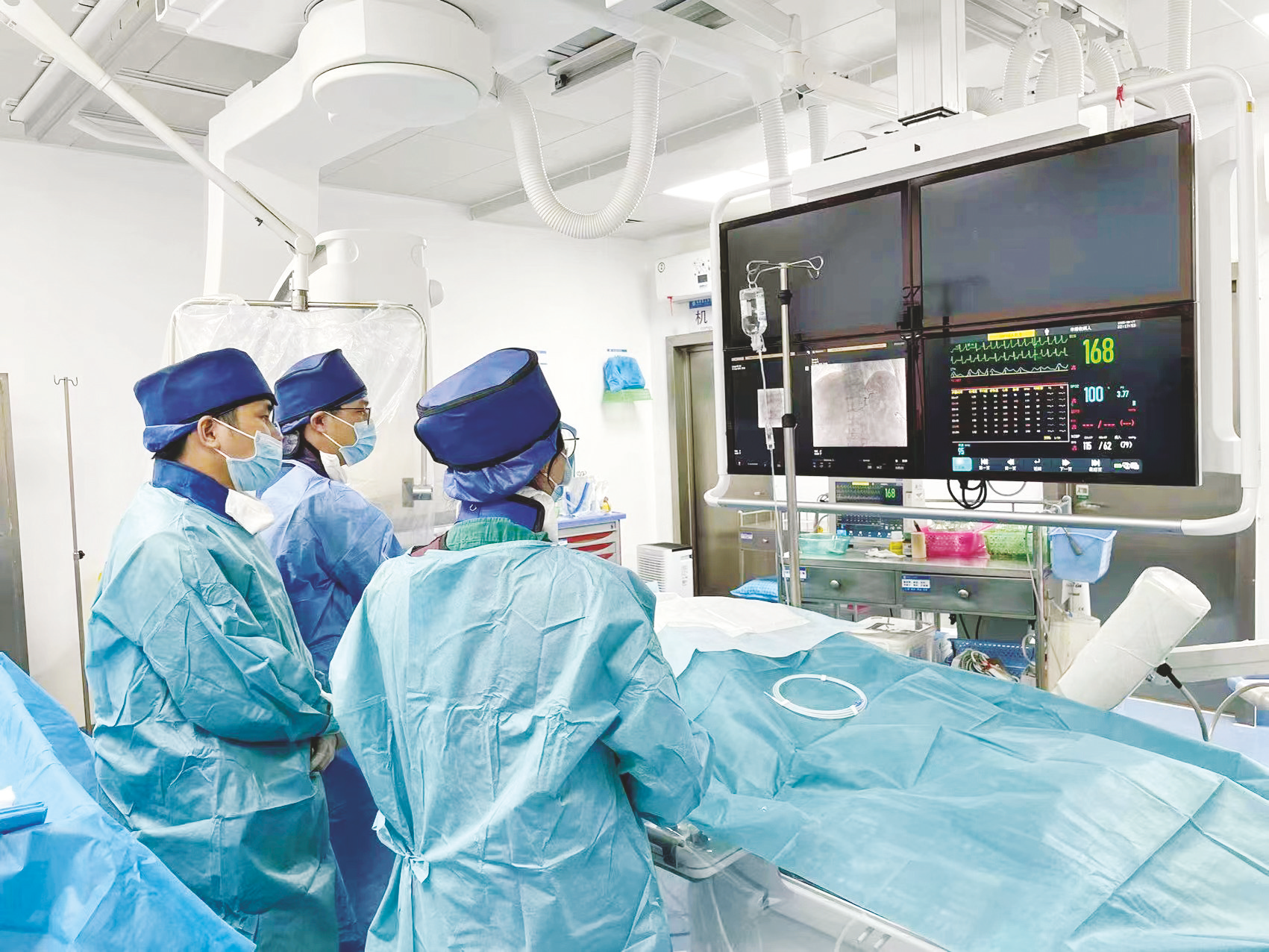
1. Interventional Therapy
Delivers drugs directly to tumor vessels via catheterization, blocking blood supply. A primary treatment for advanced liver cancer, often requiring repeated sessions.
2. Ablation Therapy
Techniques include Radiofrequency Ablation (RFA) and Microwave Ablation (MWA).
Destroys tumors with targeted heat, sparing healthy tissue.
3. CyberKnife Radiosurgery
A non-invasive alternative for inoperable, complex, or high-risk tumors.
Multidisciplinary Expertise:
U.S.-China Collaborative MDT Team: Experts from diverse specialties provide tailored treatment plans.
Complex Case Management: Over 300+ critically ill patients have received internationally advanced therapies.
Regular Tumor Boards: Held every Tuesday at 9:00 AM Beijing time for coordinated decision-making.

