
2026-03-06
During the recently concluded 2026 Spring Festival, as families gathered for reunions, a different kind of battle was unfolding in the Intensive Care Unit (ICU) of Guangzhou Fosun Chancheng Hospital (Guangzhou Xinshi Hospital), affiliated with Guangdong Pharmaceutical University—a battle to save a life against overwhelming odds.
From the initial diagnosis by Cardiology, to the robotic surgery performed by Urology, from the around-the-clock vigilance in the ICU, to the precision intervention by Interventional Radiology... This was more than a successful resuscitation; it was a powerful demonstration of the hospital's Multidisciplinary Team (MDT) approach and the unwavering commitment of healthcare professionals standing guard over life during the holiday.
A Life on the Edge: When Kidney Stones Trap a Failing Heart
Mr. Liu, 49, presented with a medical history that spanned nearly every challenging domain of medicine and surgery: coronary heart disease, acute angina, hypertension, diabetes, cardiac insufficiency, renal insufficiency, a history of cerebral infarction, and kidney stones that had troubled him for decades.
On February 2, 2026, Mr. Liu was admitted to our Cardiology Department with intermittent chest tightness for one month. Due to long-term dual antiplatelet therapy, he developed severe hematuria. The findings were alarming: his right kidney had essentially lost function due to severe hydronephrosis, while his left kidney was completely occupied by a staghorn calculus, leaving minimal renal function. His angina could not be managed conventionally due to renal insufficiency, yet his hematuria required continued anticoagulation. Mr. Liu was caught in a clinical paradox—treating one condition would exacerbate the other.
Breaking the Impasse: Preoperative MDT Forges a Safe Path, Robot Surgery Defuses the Crisis
Given the complexity, addressing the urinary obstruction to salvage left kidney function was essential before any coronary intervention could proceed. An urgent preoperative MDT meeting was convened, led by Professor Song Shengsheng, Vice President of the hospital and Director of Urology. The conference brought together specialists from Cardiology, General Surgery, Anesthesiology, Radiology, Endocrinology, Neurology, and other relevant departments. The atmosphere was focused and intense, with each expert rigorously evaluating surgical risks.
After thorough discussion, the MDT reached a consensus: given the high bleeding risk with conventional surgery, the team opted for an internationally advanced approach—Robot-Assisted Left Percutaneous Nephrolithotomy with Holmium Laser Lithotripsy. This technology integrates CT data into navigation software, automatically reconstructing a 3D model to guide precise puncture, minimizing bleeding risk and paving the way for subsequent cardiac treatment.
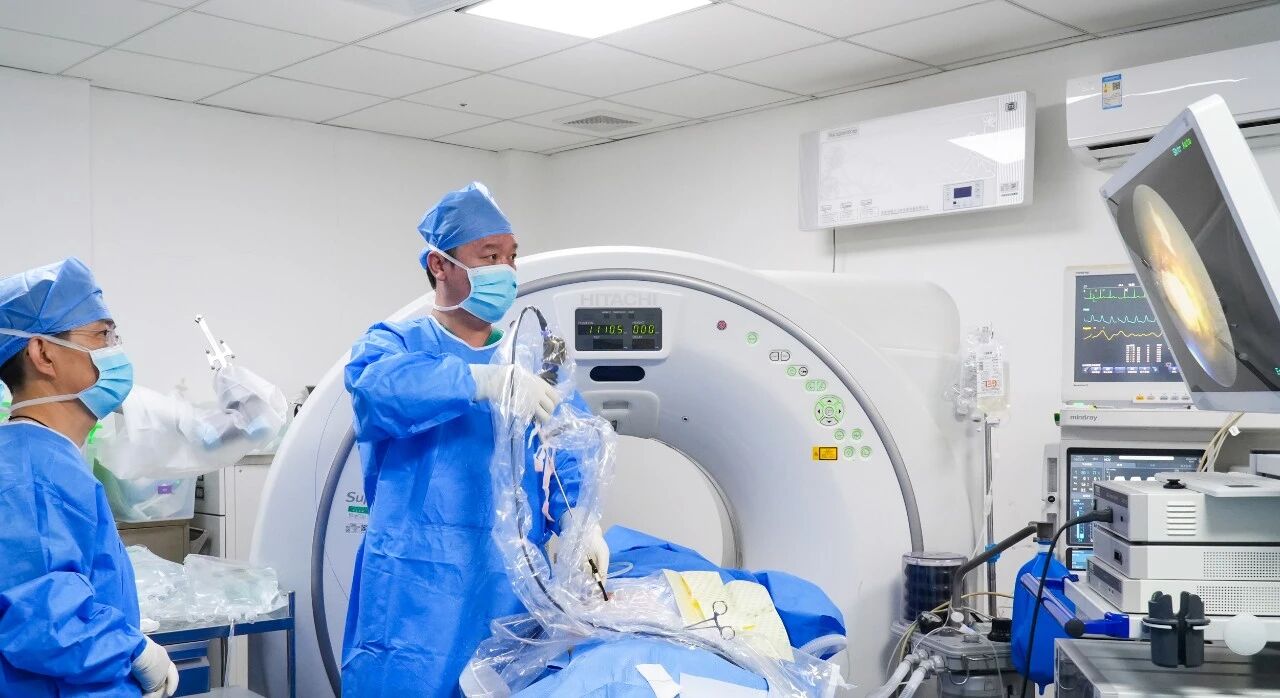
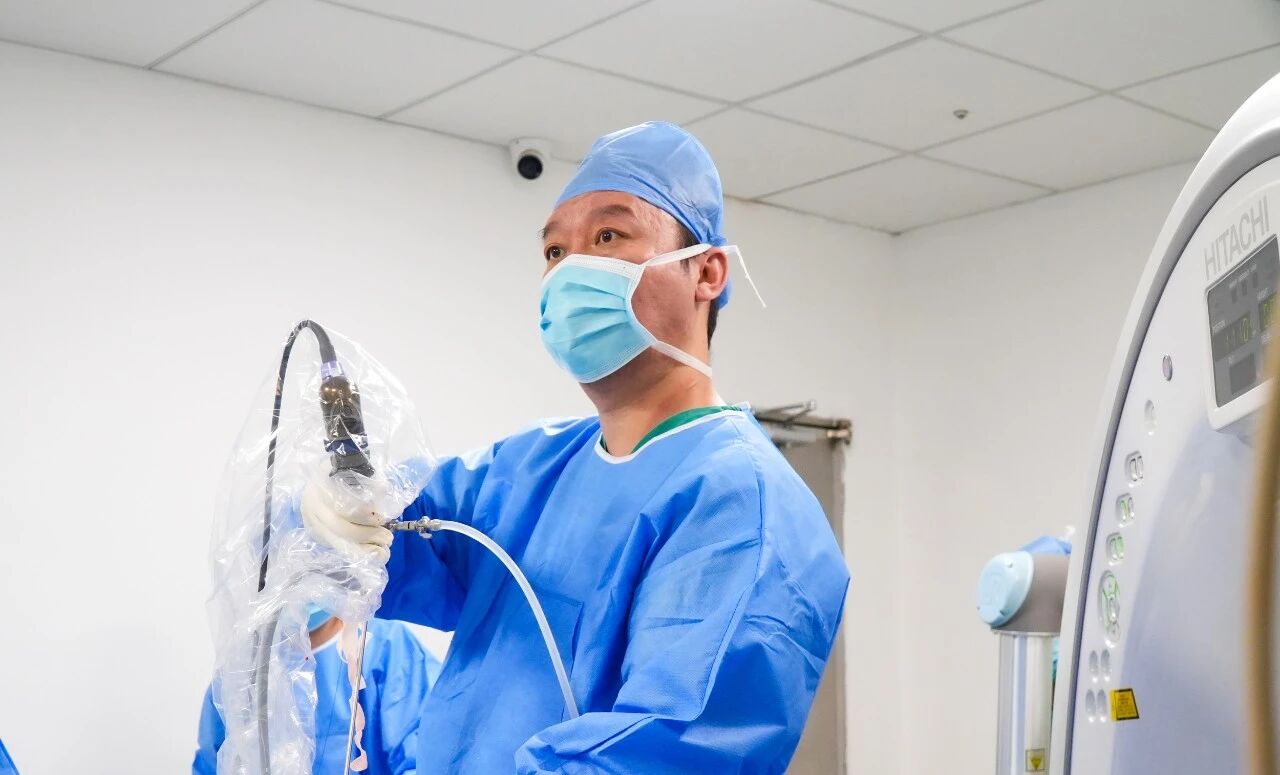
On February 10th, Professor Song performed the surgery as scheduled. Utilizing our hospital's newly acquired robotic-assisted system, he performed the left percutaneous nephrolithotomy with holmium laser lithotripsy. By importing CT data into the robotic navigation software, the system generated a rapid, intelligent 3D reconstruction—a roadmap through complex anatomy. The puncture was accurate, the targeting precise, and the staghorn calculus was successfully fragmented. To decompress the right kidney, a right percutaneous nephrostomy was performed concurrently. The first phase—clearing the obstruction—was complete.
Critical Turn: Postoperative Angina Recurrence, The ICU's Delicate Balance
Post-surgery, the patient was transferred to the ICU. But the challenges were far from over. Due to the surgical wound, antiplatelet therapy could not be resumed, and Mr. Liu's chest tightness recurred frequently. Each ST-segment depression on the cardiac monitor signaled renewed ischemia—a constant reminder of the precarious balance.
The ICU nursing team remained relentless, monitoring every ECG change, meticulously tracking cardiac enzyme fluctuations, and carefully adjusting nitroglycerin administration. Dr. Wu Yanxian, Director of Cardiology, remained on duty throughout the Spring Festival, personally visiting the ICU multiple times to guide management, engaging in bedside discussions with ICU physicians on call about navigating the narrow therapeutic window between ischemia and bleeding.
By February 12th, following medication adjustments, the patient's ECG finally normalized. The ICU team breathed easier, but all knew the underlying threat remained.
The Hidden Culprit: A Pseudoaneurysm Revealed
Just as cardiac status stabilized, a new crisis emerged. Mr. Liu's hematuria persisted, and his hemoglobin dropped to 76g/L, indicating active bleeding.
On New Year's Eve, as families prepared for celebration, Professor Song once again rallied the team: "We must locate the bleeding source—we cannot let the patient face the New Year with an unresolved threat." On February 13th, Dr. Huang Xuxin, Director of Interventional Radiology, performed renal artery angiography.

This was a procedure requiring both technical skill and patience. Angiography revealed a localized aneurysmal structure in a branch of the left renal artery, with contrast slowly filling the cavity—the source of persistent hematuria: a left renal pseudoaneurysm.
With expert precision, Dr. Huang performed superselective catheterization, deployed coils to embolize the feeding artery, and injected ONYX glue for complete occlusion. Follow-up angiography confirmed perfect sealing of the bleeding point. The life-threatening lesion was successfully eliminated.
A New Beginning: Recovery in the ICU
Following the procedure, Mr. Liu returned to the ICU, the bleeding controlled. The medical team remained vigilant, tracking every detail—from urine color to renal function recovery.
When clear urine first appeared, when hemoglobin levels steadily rose, when renal function gradually recovered after Continuous Renal Replacement Therapy (CRRT), when Mr. Liu finally slept peacefully without chest tightness—each milestone marked progress. Today, Mr. Liu is recovering well and has successfully passed the critical phase.
This Spring Festival marked the beginning of a new life for Mr. Liu. For the medical staff at our hospital, it was a vivid embodiment of their mission—revering life and healing the wounded. On this challenging journey against disease, the dedicated professionals from multiple departments, with their expertise and commitment, brought hope to a patient and his family, adding a profound meaning to the holiday season.

